MEDCINE FINAL PRATICAL (SHORT CASE)
22yr old with c/o pain abdomen
This is an online E log book to discuss our patient's de-identified health data shared after taking his/her/guardian's signed informed consent. Here we discuss our individual patient's problems through series of inputs from available global online community of experts with an aim to solve those patient's clinical problems with collective current best evidence based inputs. This E log book also reflects my patient-centered online learning portfolio and your valuable inputs on the comment box
Hall ticket no. 1701006156
CONSENT : An informed consent has been taken from the patient in the presence of the family attenders and other witnesses as well and the document has been conserved securely for future references.
DOA: 7/6/2022
A 22yr old male pt. painter by occupation resident of nalgonda came with
Chief Complaints:
Pain abdomen since 4 days.
HOPI:
Pt. Has started consuming alcohol 4 yrs back due to peer pressure , intially taking one peg per day which has increased to 90ml morning and evening i. e twice daily. He has stopped consuming alcohol 3 months back as advised by the doctor.
Pt. Has history of smoking since 2 yrs . He has been smoking beedies 5 per day till date.
Pt was apparently asymptomatic 3 months back then he developed abdominal pain which was dragging in character for which he was admitted in near by hospital in nalgonda . He was diagnosed with acute pancreatitis and was treated inadequately and was advised to stop consumption of alcohol.
Since then pt has stopped consuming alcohol and has been experiencing alcohol withdrawal symptoms like getting angry , agitation , irritability , craving to consume alcohol, tremors . Pt had consumed alcohol 4 days back due to family problems.
In veiw of this symptoms pt.has been brought to psychiatry OPD for deaddiction. He was referred to medicine OPD in veiw of pain abdomen.
Pain was , insidious in onset , started after consuming of alcohol in epigastrium and left hypochondrium which was relieved on bending forward and lying down , aggrevated on eating food and standing straight.
No h/o fever , nausea , vomiting.
Past history:
H/o similar complaint in past 3 months back.
No other co morbid conditions
No h/o previous medical surgical history.
Family History
Not significant
Diet : mixed
Appetite : normal
Bowel bladder: regular
Sleep: inadequate
GENERAL EXAMINATION
Pt was concious coherent and cooperative
Thin built and moderately nourished
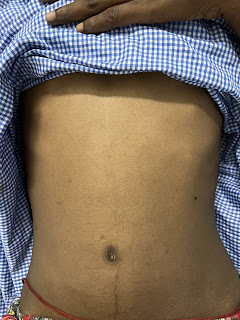
ABDOMEN
No icterus,cyanosis , clubbing,lymphadenopathy, edema
Vitals
Temperature- afebrile
Pulse rate-94bpm
Blood pressure-120/80mmHg
Respiratory rate- 16cpm
Systemic examination:
Abdominal examinations:
Inspection:
Okay Shape of the abdomen- flat
Umbilicus is central
No visible scars,pulsations, peristalsis, engorged veins
Palpation:
All the inspectory findings are confirmed.
Tenderness present over the epigastrium region
No organomegaly
Percussion
No free fluid
Ascultation:
Bowel sounds heard
Other systems:
Respiratory:
b/l air entry present , no added breath sound
CVS :
S1 S2 heard , no added murmurs
CNS :
Higher function intact
No motory and sensory deficit.
Cranial nerves normal .
Investigations
Complete blood picture
Complete urine examination
RFT
USG abdomen
Serum amylase
Serum lipase
Diagnosis:
acute pancreatitis.
TREATMENT
Nil per oral
IV fluids Ringer lactate
,Normal saline 100 ml per hour
Inj. Tramadol100mg in 100ml NS IV BD
Inj.pantop 40 mg IV OD
Inj. Optineuron 1 ampoule in 100ml NS IV OD
Psychiatry medication
Tab . Lorazepam 2mg BD
Tab . Benzothiamine100mg OD
12/06/22 FOLLOW UP
VITALS
pulse rate: 92 bpm
BP: 110/70mm of hg
Temp: afebrile
CVS: S1S2 heard
CNS: NAD
Lungs: BAE+
TREATMENT
IV Fluids RL/NS at the rate 75/min
Allow soft diet orally
Continue same medications as above